 The physical exam – looking into the eyes and throat, taking the blood pressure, sounding the chest – is part of the process of medical diagnosis. It’s one way a physician attempts to determine the cause of a patient’s complaint.
The physical exam – looking into the eyes and throat, taking the blood pressure, sounding the chest – is part of the process of medical diagnosis. It’s one way a physician attempts to determine the cause of a patient’s complaint.
In recent times, doctors have asked themselves whether the physical exam is becoming a lost art. It’s been replaced by an array of laboratory tests and high tech machines that presumably provide greater accuracy than the eyes, ears, and touch of a mere human being. (Smell, of course, also provides clues, and device makers are inventing medical gadgets that detect scents. Doctors no longer taste urine for sugar, as they did from antiquity into the 19th century, nor do they taste perspiration to see if it’s sweet, salty, or acrid.)
The reasons for the current decline of the physical exam are many. Hospital stays used to be much longer, so students had more time to learn from patients. The modern resident’s work week is officially limited, so there’s less time to spend at the bedside. Office visits are now much shorter, and a hands-on exam uses precious time.
The physical exam could completely fade away. It could become a staple only of certain specialties. Or – if it’s viewed as an important component of the doctor-patient relationship – it could experience a renaissance. Its future remains to be seen.
What’s not widely known, however, is that this is not the first time the physical exam has gone into decline. We know from surviving medical treatises that the exam was an integral part of a physician’s practice in ancient Greece and Rome. This continued to be true until the late Middle Ages (1300-1500). The hands-on exam then disappeared for hundreds of years, reemerging gradually in the late 18th century.
There were a number of reasons for this decline, including changes in medical education, a desire on the part of educated physicians to occupy an elite position in society, and a lowering of the social standing of surgeons. A brief look at this previous disappearance illustrates how the practice of medicine is very much a product of the social climate in which it exists.
Hippocrates, Galen, and the humoral theory of disease
We know from the Hippocratic Corpus (fifth to third centuries BC) that physicians were advised to dismiss supernatural causes of disease and concentrate on empirical evidence. “It is the business of the physician to know in the first place, things … which are to be perceived by the sight, touch, hearing, the nose, and the tongue, and the understanding.” We know, for example, that Hippocratic physicians palpated the abdomen and thorax. Understanding meant knowing the individual patient as a whole person. To diagnose, one needed to learn the patient’s habits, way of life, work, diet, etc.
The Hippocratic school held that the body was filled with four fluids – blood, yellow bile, black bile, and phlegm – and that these fluids could become unbalanced. Blood-letting, for example, was a way to rebalance an excess of blood. This theory of the composition and workings of the human body was called humoralism.
Galen, a prominent physician who practiced in Rome in the second century AD, continued the Hippocratic tradition of humoralism, adding a greater emphasis on anatomy, physiology, pathology, and logic. He performed dissections — and vivisections – of animals (autopsies were illegal). When Galen palpated the abdomen, he knew the location of the liver, spleen, and bladder. He examined stool samples for color, consistency, and composition. Like his Hippocratic predecessors, he reportedly spent many hours in conversation with a patient as a means of reaching a diagnosis.
We know about Galen’s practices because he left a large corpus of texts that was studied by medical students well into the 19th century. It’s Galen’s theory of pathology – the study and diagnosis of disease – that dominated medicine for almost 2000 years.
Both Hippocrates and Galen were physician-philosophers – theoreticians – but they were also craftsmen. They worked not only with their minds, but with their hands, both to diagnosis illness and to perform surgery. Surgery included the treatment and bandaging of wounds, and, in the case of Galen, procedures performed on the brain (to relieve pressure) and eyes (cataracts). There was, of course, no internal surgery, although there were occasional exceptions, such as removing a bladder stone.
Med school reform and the disappearance of the physical exam
Galen’s teachings were lost when the Western Roman Empire collapsed in 476. They were preserved in Arabic, however, in the Eastern Roman (Byzantine) Empire. Beginning in the 11th century, Galen’s works were translated back into Latin and, by the late Middle Ages, became the basis of western medical education.
A profound change happened at this time – a change that explains the loss of the hands-on physical exam. Medical practitioners separated into physicians and surgeons. Physicians were literate, read (and spoke) Latin, and acquired their medical training in universities. Surgery became a manual craft, learned by apprenticeship. Where previously the theories of the physician and the practical skills of the surgeon had been combined in one practitioner, medicine and surgery were now separate. Physicians were highly regarded by society for their book learning, and surgeons occupied a much lower social standing.
This is when physicians – with a few geographic exceptions – stopped practicing the hands-on physical exam. Scholarship was valued over sensory experience. Reason took precedence over observation. The educated physician valued mental activity and distained manual labor.
In making a diagnosis, the physician gave priority to the patient’s account of his or her symptoms, even if it contradicted what the physician observed with his own eyes. (There were no women physicians, of course.) Patients could be diagnosed through the mail, just as Abraham Verghese writes today about the iPatient who can be diagnosed from electronic medical records with only a cursory visit to the bedside.
The relative social standing of physicians and surgeons
Surgeons became the primary care physicians of their day, attending to patients who could not afford the more expensive physicians. Since this class of patients couldn’t pay very well, surgeons almost always practiced another profession. Commonly they were barbers, but also innkeepers, and later apothecaries (today’s pharmacists).
Educated physicians sought patients among the well-to-do upper classes. Although physicians were more respected than surgeons, they were not necessarily of the same social status as their patients. They aspired to be dignified gentlemen, however, which meant they would not demean themselves by engaging in manual labor. When the stethoscope was first introduced, it was opposed by physicians who viewed its use as a manual procedure. When thoracic percussion was introduced, the response was indifference. Physicians did not handle the bodies of their patients directly.
What physicians did do was observe the general appearance of the patient (especially the face) and note behavior. They took the pulse, not for its speed, but for its quality (similar to traditional Chinese medicine). They examined urine, stool, sputum, and pus, since those specimens provided clues to the internal humors.
By the 17th century, there were thermometers that could measure a patient’s body temperature. Physicians could not find a relation, however, between temperature measurement and a patient’s subjective sense of warmth – a patient could have a fever, but feel chilled. So this new information was considered to be of no particular value.
The advent of scientific medicine
The physician’s resistance to working with his hands or using his senses to make a diagnosis, as Hippocrates and Galen had done, was not just obstinacy or social climbing. It made sense given the humoral theory of the body. Because illness was considered a unique imbalance in each individual, the patient’s account of his or her disease took precedence over what a physician could observe. There were as many diseases as there were patients. There was not yet a concept of the local origin of disease in specific organs or tissues. In humoral theory, diseases could move from one site in the body to another.
In the 18th century, medical education began to associate itself with newly established hospitals, which primarily served the poor. These hospitals provided medical professors and their students with the opportunity to correlate the symptoms of a living patient with evidence revealed by autopsy after death.
This was the beginning of the end for humoralism, which was gradually replaced by the scientifically based medicine we know today. Physicians and surgeons began to attend the same schools and study the same subjects. The sharp division between the two practices began to erode. Once medicine acquired this new understanding of disease, doctors wanted to know as much as possible about the internal state of the body. The hands-on physical exam, aided by new technologies such as the stethoscope, made a comeback.
Fluctuating attitudes towards physicians in the 19th and 20th centuries
Has the rise of scientific medicine had an impact on the social status and professional regard for physicians in our own time? Most definitely.
In 19th century America, there were elite physicians in the big cities – Boston, New York, Chicago – whose patients could afford to pay handsomely. For the rest of the medical profession, incomes were quite meager. Becoming a doctor, however, was a ticket to respectability. A poor boy could apprentice to an experienced physician and become a member of the middle class. (For a woman to be a doctor was quite exceptional at this time.)
Once medicine changed from humoralism to a scientific theory of disease – especially once medicine had something to offer by way of treatment and not just improved diagnosis and prognosis – the prestige of the medical profession was greatly enhanced. Doctors acquired the same status as scientists, who were held in high regard. Vaccines and microbiology brought infectious diseases under control. By the mid-twentieth century, wonder drugs had ushered in the Golden Age of medicine for both patients and physicians.
The Golden Age was all too brief, for patients and ultimately for physicians too. Rapid advancements in pharmacology and high tech imaging in the second half of the 20th century turned medicine into biochemistry and radiology. No longer was medicine primarily the healing art it had been traditionally. Who needs the time-consuming doctor-patient relationship in an era of penicillin, Prozac, and positron emission tomography.
From doctor-patient relationship to medical encounter
Both the physical exam and attentive listening to the patient’s history had provided psychological benefits which were at the core of the doctor-patient relationship. As both disappeared, those benefits were lost. Patients responded with anger, alienation, withdrawal, and disloyalty. They felt free to initiate malpractice suits and to spend more of their own out-of-pocket money on alternative care than on conventional medicine.
In the 1970s, there was a school of thought that argued medicine was turning people into lifelong patients and doing more harm than good. As Edmond Shorter points out
, it’s ironic that, just when medicine finally began to offer life-saving treatments, public regard for the medical profession declined.
It’s not that individual doctors, who were still the same sympathetic human beings they’d been throughout the ages, cared any less about their patients. But the expression of concern for the patient – taking time to know the whole person – was no longer therapeutically essential. The Golden Age of medicine, with its amazing scientific discoveries that turned physicians into demi-gods, ended abruptly when patients stopped worshipping. Medicine became a business and the physician/surgeon just another businessperson.
That’s a bit of an overstatement, I admit. Patients still trust their doctors, and medicine is still a highly respected profession, but there’s a grain of truth there. The change in vocabulary speaks volumes. The “doctor” has become a “provider,” the “patient” is now a “client” or “consumer,” and a “visit” with your doctor – a term that suggests conversation at least, if not the serving of tea – is now a “medical encounter.”
Related posts:
The doctor-patient relationship: What have we lost?
The esteem of the medical profession: Then and now
The physician as humanist
The art and science of medicine
Marcus Welby vs. the specialists
Physician as lone practitioner
Resources:
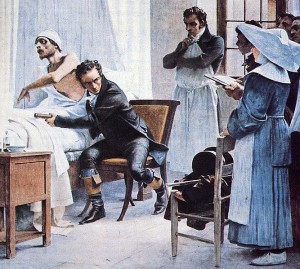
Image: Wikipedia. Physician Rene Laennec (1781-1826) examines a consumptive patient with a stethoscope in front of his students at the Necker Hospital, a teaching hospital in Paris. Painting by Théobald Chartran, 1816.
Jill Max, The lost art of the physical exam, Yale Medicine, Winter 2009
Lisa Sanders, Every Patient Tells a Story: Medical mysteries and the art of diagnosis
Malcolm Nicolson, The Art of Diagnosis: Medicine and the Five Senses, in Companion Encyclopedia of the History of Medicine, edited by W.F. Bynum and Roy Porter, pp 801-825
Roy Porter, The rise of physical examination, in Medicine and the Five Senses, edited by W.F. Bynum and Roy Porter, pp 179-197
Abraham Verghese, Culture Shock — Patient as Icon, Icon as Patient, The New England Journal of Medicine, December 25, 2008 (subscription required) Available as a PDF here.
Richard Reece, Why doctors should profit from dispensing medications, KevinMD, January 15, 2011
Kevin Pho, iPatients and the demise of the bedside physical exam, KevinMD, December 27, 2008
Kevin Pho, Are doctors finding the physical exam useless and obsolete?, KevinMD, January 2, 2009
Robert Centor, Many doctors order tests rather than do a history and physical, KevinMD, September 25, 2010
Edward Shorter, The History of the Doctor-Patient Relationship, in Companion Encyclopedia of the History of Medicine, edited by W.F. Bynum and Roy Porter, pp 783-800
Edward Shorter, Bedside Manners: The Troubled History of Doctors and Patients
Ghislaine Lawrence, Surgery (Traditional), in Companion Encyclopedia of the History of Medicine, edited by W.F. Bynum and Roy Porter, pp 961-983
Susan Lawrence, Medical Education, in Companion Encyclopedia of the History of Medicine, edited by W.F. Bynum and Roy Porter, pp 1151-1179


Hello Jan,
This is absolutely fascinating – thank you so much for this. You have somehow managed to make the history of the physical exam both concise yet compelling.
And your description of the evolution of the medical “encounter” sums up, certainly from a patient’s perspective, the growing divide between ‘them’ and ‘us’.
Not all of these encounters happen just between patient and physician, of course. Many equally distressing encounters happen when patients meet a health care professional assigned to do a diagnostic procedure on us. Depending on the day, the personality of the tech, the burn-out factor, the tedium of repetitious test after test after test, the standards of quality care demanded by individual supervisors – enduring routine diagnostics can become, surprisingly, one of the most upsetting procedures patients talk about.
I wrote recently about the brutal disconnect of such “encounters”, in an open letter to hospital employees after a particularly distressing stress echocardiogram procedure after my heart attack, in which I politely offer my “Top 10 Tips For How To Treat Your Patients”. It’s at Heart Sisters: http://myheartsisters.org/2009/07/10/open-letter/
I also enjoyed your very wise recent comment on kevinmd.com.
Cheers,
C.
Thanks for your comment, Carolyn. It’s interesting to hear about the distress generated by the total health care encounter. I enjoyed the post you reference at Heart Sisters. With regard to your points 6 through 10 in that post, which touch on the subject of patient modesty, I recommend the relatively new blog, Patient Modesty & Privacy Concerns (http://patientprivacyreview.blogspot.com/). They are open to guest bloggers, and I’m sure they would appreciate hearing what you have to say.
I’m also very sympathetic to the topic of your other blog, The Ethical Nag (http://ethicalnag.org/). I too have been infuriated by revelations about the lack of ethics in the pharmaceutical and medical device industries (not to mention the granddaddy, tobacco). Recently there have been some interesting developments that take the subject to a whole new level. What’s being questioned is not so much a lack of ethics, but the fundamental assumptions about how science is done these days.
One example is the reaction to Jonah Lehrer’s article, The Truth Wears Off, in the New Yorker (http://nyr.kr/eJbi71). Another is reactions to an article proving the existence of ESP, published in a reputable psychology journal (NYT story at http://nyti.ms/fZZKQd). These developments were preceded by David Freedman’s article in The Atlantic (Lies, Damned Lies, and Medical Science) (http://bit.ly/hTI9hN), based on his book, Wrong: Why experts* keep failing us — and how to know when not to trust them. I touched on this in connection with preventive health care in a post a few months ago (http://bit.ly/fYAsAF). Not only are there grounds for lacking confidence in the prescriptions we take, but for following advice on disease prevention based on purportedly scientific evidence.
As you write in your description of The Ethical Nag, patients are taking pills based on tainted research because physicians trust what’s published in journals. We know what happens when research is financed by drug companies, plus there are all those other outrageous shenanigans that come out in whistle-blower lawsuits. These latest accusations point to something even more disturbing than publication bias.
In the 1990s, social scientists and intellectuals in the humanities attacked science from a social constructionist point of view – the idea that scientists were unaware of biases that stem from the social and economic system in which they’re embedded. Scientists were able to pooh-pooh that, and it blew over. These new criticisms strike at the assumptions of mathematical statistics that are at the foundation of clinical trials. Scientists are taking this more seriously, I believe.
I enjoyed your comments on KevinMD, also. (Why doctors should profit from dispensing medications — http://bit.ly/hkADJt) The overall response of doctors to that post supports the idea that doctors see themselves as businesspeople these days. It’s sad that doctors in private practice are reduced to marketing drugs and promoting the use of their in-house imaging equipment. It’s not good for patients, and it’s not good for health care costs. It’s a new low in the history of the medical profession. I don’t blame the profession — except for spending way too many decades resisting universal health care. What’s happened to medicine is the result of the bureaucratic/economic times we live in.